服務介紹
台灣40歲以上成人巨細胞病毒帶因率高達七成以上,但此病毒跟感冒一樣,有許多不同的變異,即使準媽媽孕前已經感染過某一型的巨細胞病毒,仍可能於懷孕中感染新種類病毒株,而導致新生兒先天性巨細胞感染。 據統計,台灣平均每年有3,600個新生兒感染先天性巨細胞病毒 ,更有8%的先天性聽損寶寶是肇因於此一疾病。
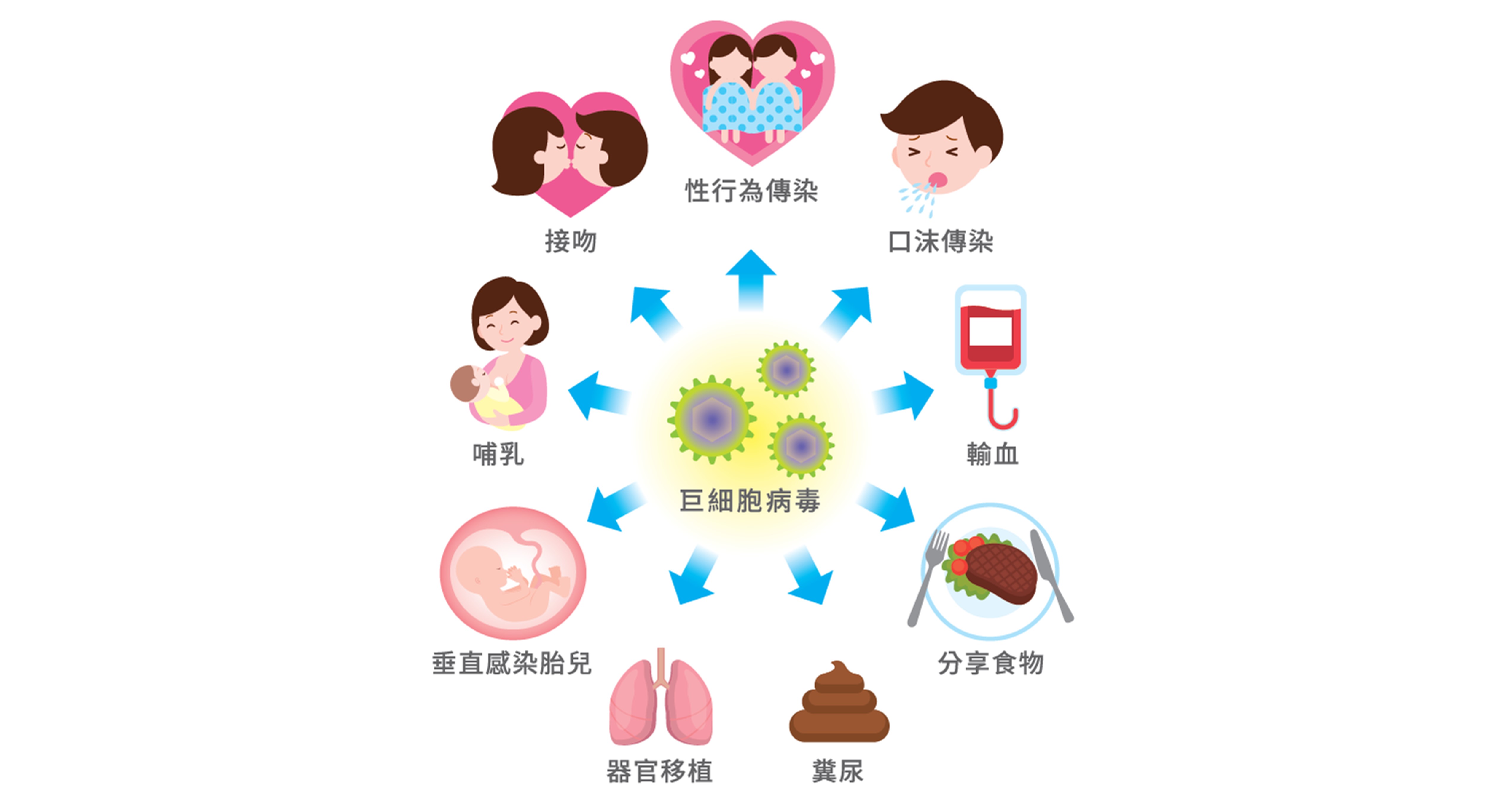
■ 每個看起來健康的正常人 都可能是巨細胞病毒的傳播者
巨細胞病毒是台灣最常見的病毒感染之一,絕大多數的受感染者都沒有明顯症狀,但感染後病毒會終身潛伏,且有機會傳染給其他人,一旦免疫力因嚴重燒傷、重大疾病、器官移植等因素驟降時,病毒也可能再次活化引發嚴重病症。
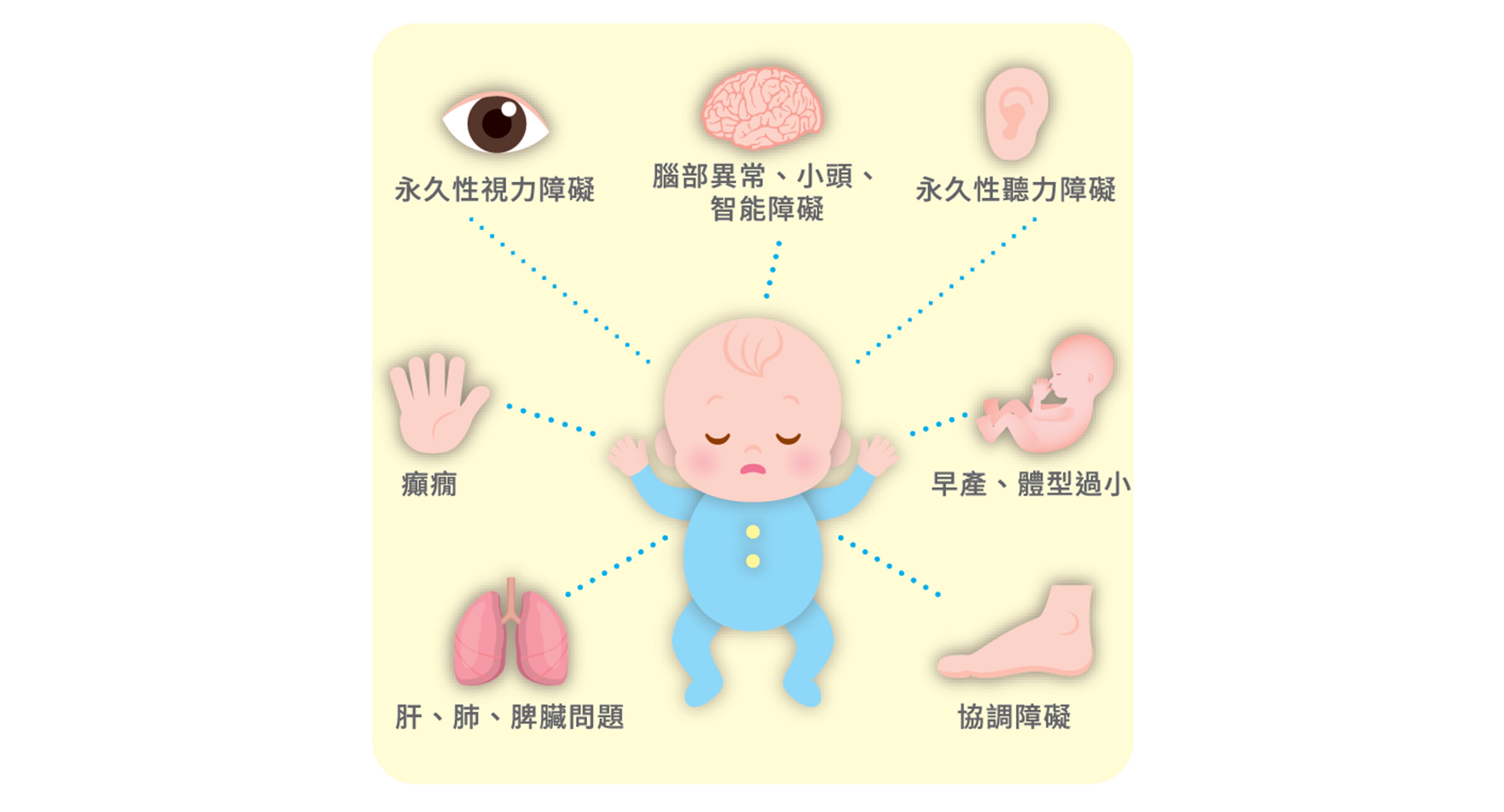
對於未出生的寶寶來說,巨細胞病毒卻是非常可怕。若媽媽曾經感染過巨細胞病毒,帶有可以保護寶寶的抗體,問題還不大,大部份的小孩都可以健康出生長大;若於懷孕中才初次感染巨細胞病毒,沒有抗體保護的寶寶就有機會透過胎盤垂直感染,造成許多嚴重問題,甚至在出生數天或數周後死亡。這些症狀可能在出生之時就發生,也有機會在數年後才慢慢出現,而且由輕加重逐步惡化。
■ 早期診斷與治療:降低先天性巨細胞病毒感染後遺症風險
過去大家普遍認為先天性巨細胞病毒感染無藥可醫。寶寶在出生前就已經感染,絕大部份沒有症狀。有症狀的,傷害已經造成,想治療恐怕來不及。
近年來發現出生時看似健康的寶寶可能陸續出現聽損等情形,有症狀的人症狀可能加重,表示病毒對身體的傷害仍在進行中,也陸續有新藥物開發出來,給予治療更多可能性。若確認寶寶已感染,可在專業醫師指導下使用抗病毒藥物以降低症狀惡化機率。
檢測說明
‧ 為區分先天性子宮內感染和出生後感染,必須在寶寶出生兩周內盡快採集血液測試其中是否含有病毒DNA,超過兩周後則難以區別。
‧ 建議搭配例行性新生兒先天性代謝異常疾病篩檢一起進行,寶寶不用多扎針,卻得到更多健康保護。
適用對象
符合以下條件之新生兒:
✔ 母親沒有做過巨細胞病毒篩檢
✔ 母親懷孕前或懷孕中曾做過巨細胞病毒篩檢,篩檢結果為陰性(未曾感染巨細胞病毒)但生活中有可能接觸到巨細胞病毒
✔ 母親確定曾感染過巨細胞病毒,擔心寶寶仍有機率垂直感染
✔ 母親為褓姆、幼稚園老師、護理人員等有較高機會受到巨細胞病毒感染者
檢測流程
步驟一: 在專業的諮詢人員講解下,更進一步了解新生兒基因檢測,並完整填寫新生兒基因檢測同意書
步驟二: 寶寶由醫護人員進行腳跟血採集,並將採集好的新生兒血片,運送至慧智進行新生兒基因檢測
步驟三: 兩星期後寄送新生兒基因檢測報告至院所,並由專業醫師解說新生兒基因檢測報告結果
其他說明
個案分享
晴晴(化名)出生的時候哭聲宏亮,非常健康,接受新生兒聽力篩檢也顯示一切正常。但在兩歲時被診斷出重度聽損,經追蹤診斷發現聽力情形逐漸惡化,最後助聽器已經不足以輔助,需要使用電子耳。
抽血檢驗結果顯示,晴晴體內帶有巨細胞病毒。如果晴晴可以在出生時就檢驗是否有感染,再配合專業醫師及早對症下藥,也許可以保留更多的聽力。
